Stay Updated with Wellness Digestive




No spam, no fluff—just practical, evidence-based advice delivered straight to your inbox every Tuesday.







If you live with IBS, you may have noticed something frustrating: one bad night of sleep… and the next day your gut feels louder. More bloating. More urgency. More cramping. More sensitivity to food.
That connection is not coincidence. Sleep and IBS are linked through circadian rhythm timing, stress hormones (including cortisol), gut motility patterns, and the gut–brain axis. When sleep is disrupted, those systems become less coordinated – and your digestive system often pays the price.
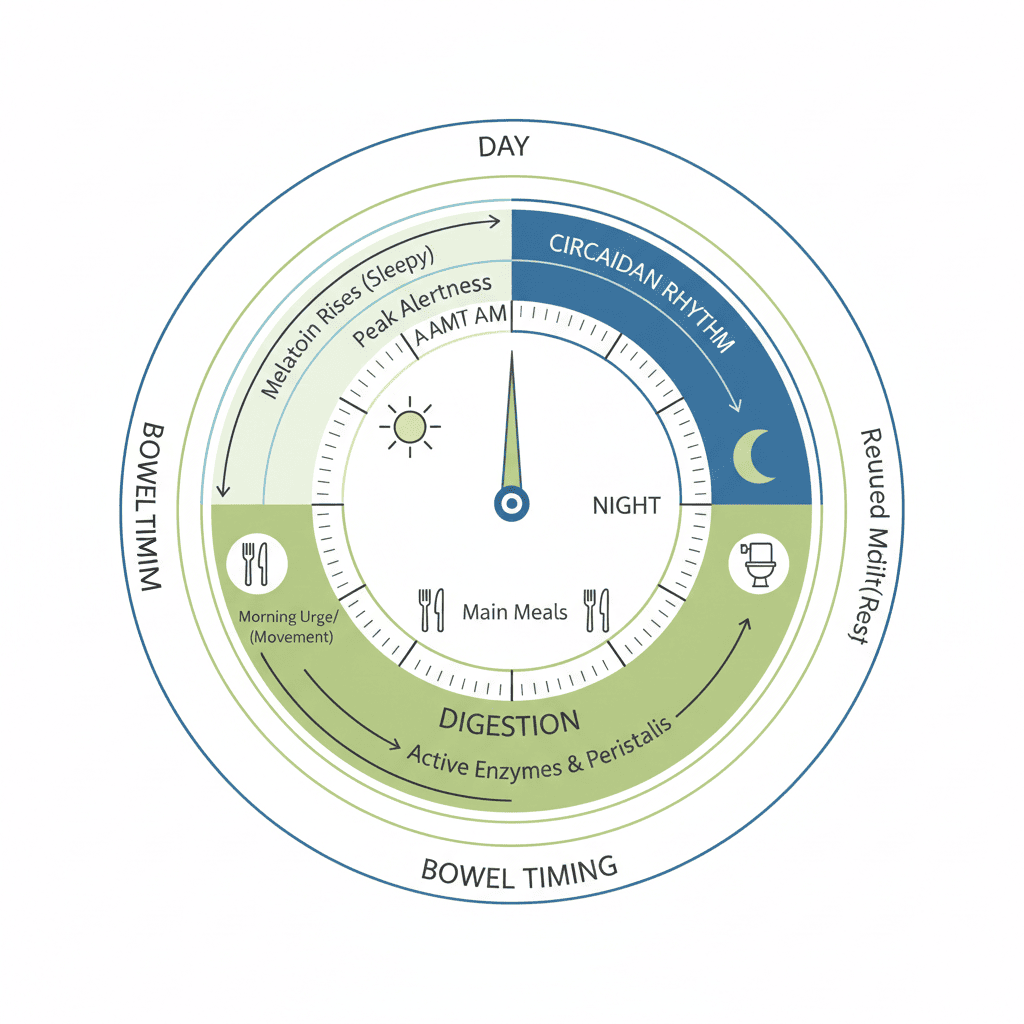
Your body runs on a 24-hour internal rhythm called the circadian rhythm. It helps regulate sleep–wake cycles, cortisol release, digestive secretions, and daily patterns of gut motility and bowel timing.
Your brain has a “master clock,” but your gut has its own peripheral clock too – which means digestion doesn’t happen randomly. It follows daily rhythms. When sleep is irregular, those rhythms can get disrupted, and IBS symptoms can flare.
For a clear overview of IBS and how multiple body systems play a role, see the NIDDK resource: Irritable Bowel Syndrome (NIDDK).
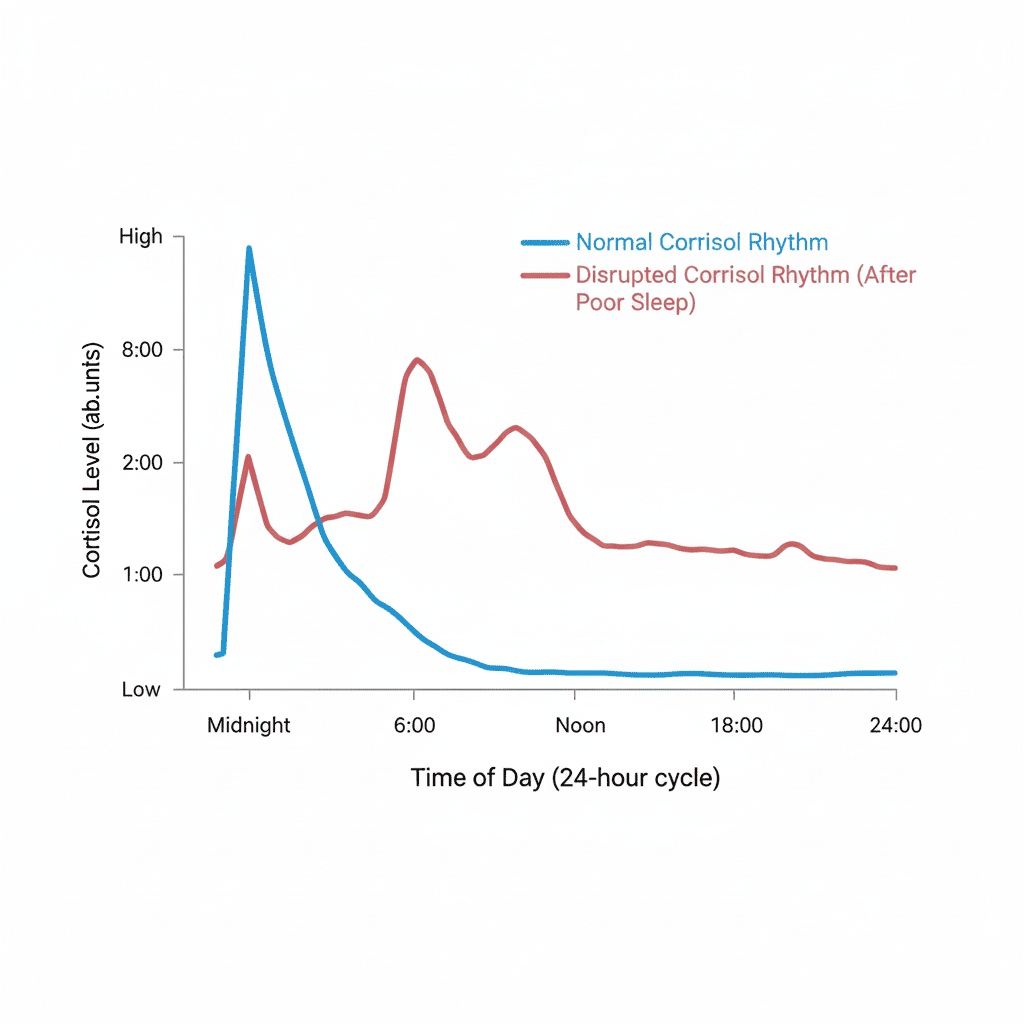
Cortisol normally follows a daily rhythm: higher in the morning to help you wake up, then tapering through the day, lowest at night to support sleep. Poor sleep can disrupt that rhythm. When cortisol becomes dysregulated, gut sensitivity and stress reactivity tend to rise – which can make IBS symptoms feel stronger the next day.
Sleep loss lowers pain threshold. In IBS, where visceral hypersensitivity is common, that matters. A normal amount of gas or bowel pressure can feel more uncomfortable after a poor night.
Circadian disruption can affect motility patterns, which may lead to less predictable bowel movements. For IBS-C, poor sleep can contribute to slower transit. For IBS-D, stress-related sleep disruption can intensify urgency. The same disrupted system can push symptoms in different directions depending on your subtype and baseline pattern.
Sleep is when your nervous system recalibrates. Chronic sleep disruption increases sympathetic (“fight-or-flight”) tone and reduces recovery time – which can reduce resilience and make stress-triggered gut symptoms more likely.
Johns Hopkins has a helpful IBS overview that includes the role of stress and lifestyle factors: IBS overview (Johns Hopkins Medicine).
It often looks like this:
Breaking the cycle doesn’t require perfection – it requires small, consistent adjustments.
You don’t need a two-hour bedtime routine. You need rhythm and predictability.
If you change only one thing, change this: wake up at roughly the same time every day – even after a poor night. Wake time anchors your circadian rhythm and supports more stable cortisol timing the next day.
Light is one of the strongest signals for your circadian clock. Try 5–15 minutes of outdoor daylight in the morning. This supports healthier sleep timing and may help regulate daily digestive rhythms.

Also consider meal timing: many people feel better when dinner ends 2–3 hours before bed (when feasible).
Try not to escalate the moment into panic. Instead:
If abdominal pain wakes you regularly, talk with your clinician about nighttime symptom management, caffeine timing, meal timing, and whether your fiber or medication timing needs adjustment.
For an evidence-based overview of IBS treatments (including medications and behavioral approaches), see the ACG guideline: ACG Clinical Guideline: Management of IBS.
Seek medical evaluation if you have frequent nighttime diarrhea, blood in stool, unexplained weight loss, or severe pain waking you nightly. IBS can affect sleep, but red-flag symptoms deserve medical review.
Sleep is not just rest – it’s hormonal calibration, nervous system reset, immune regulation, and digestive rhythm stabilization. If your IBS worsens after poor sleep, your body isn’t failing. It’s responding to disrupted regulation.
Start small:
Your gut loves rhythm – and sleep is one of the most powerful rhythms you can protect.