Stay Updated with Wellness Digestive




No spam, no fluff—just practical, evidence-based advice delivered straight to your inbox every Tuesday.






Diagnosing Irritable Bowel Syndrome (IBS) is a bit like piecing together a puzzle. The symptoms can overlap with other gastrointestinal conditions, making it tricky to pinpoint the cause. The good news is that IBS is diagnosed using a set of clear clinical criteria, which can help you understand your symptoms and manage your treatment more effectively.
The Rome IV criteria are widely considered the gold standard for diagnosing IBS. But understanding what these criteria really mean can be confusing-especially if you’re not familiar with medical terminology. That’s why we’ve broken it down for you in simple terms.
Irritable Bowel Syndrome (IBS) is a chronic digestive disorder that affects the large intestine. It’s one of the most common gastrointestinal disorders, causing symptoms such as:
Unlike other conditions like inflammatory bowel disease (IBD), IBS does not cause permanent damage to the digestive tract, and it does not increase the risk of more serious diseases like cancer. Instead, it is a functional disorder, meaning there’s no structural issue with the bowel itself, just a dysfunction in how the bowel works.
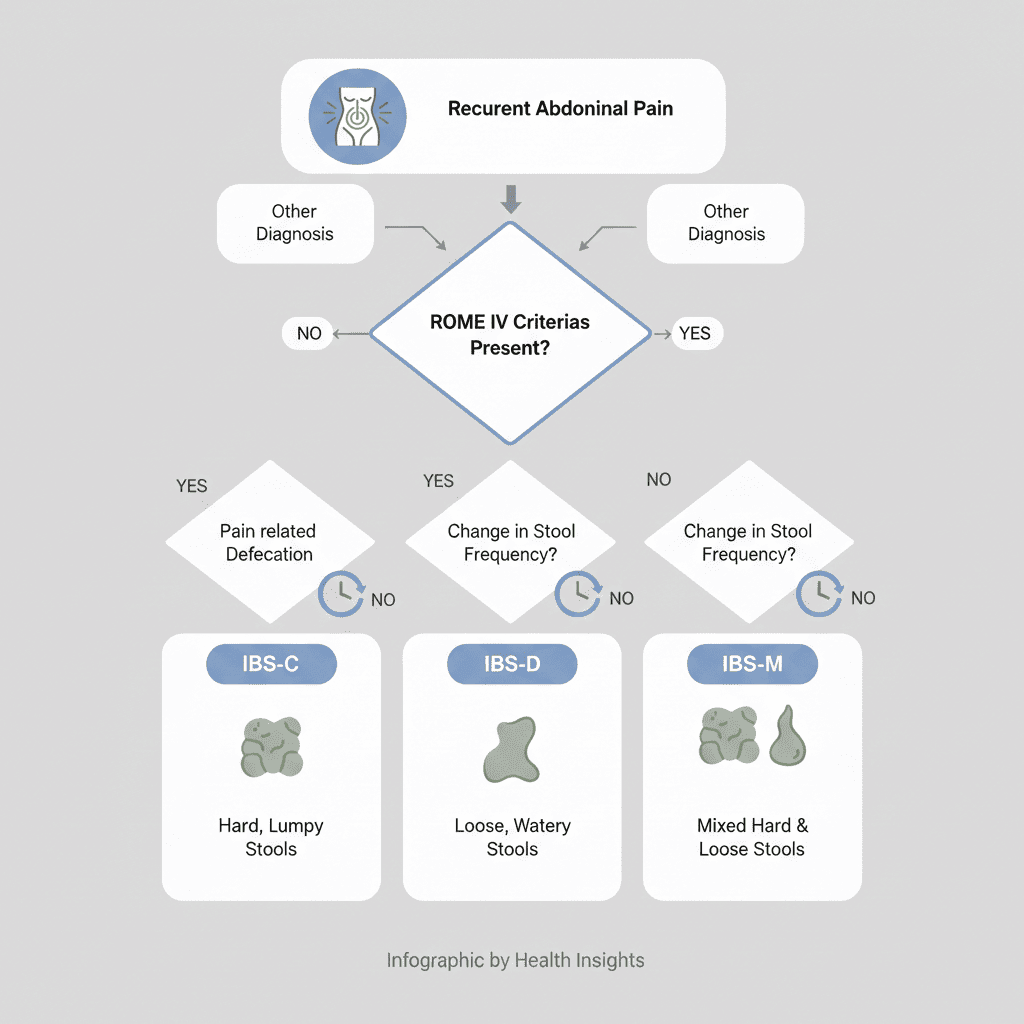
The Rome IV criteria are the most widely accepted diagnostic system for IBS. They were developed by the Rome Foundation, a leading group of medical experts focused on functional gastrointestinal disorders.
To meet the Rome IV criteria, a person must experience recurrent abdominal pain at least one day per week for the past three months, associated with two or more of the following:
These symptoms must also have been present for at least 6 months before a doctor can confirm an IBS diagnosis.
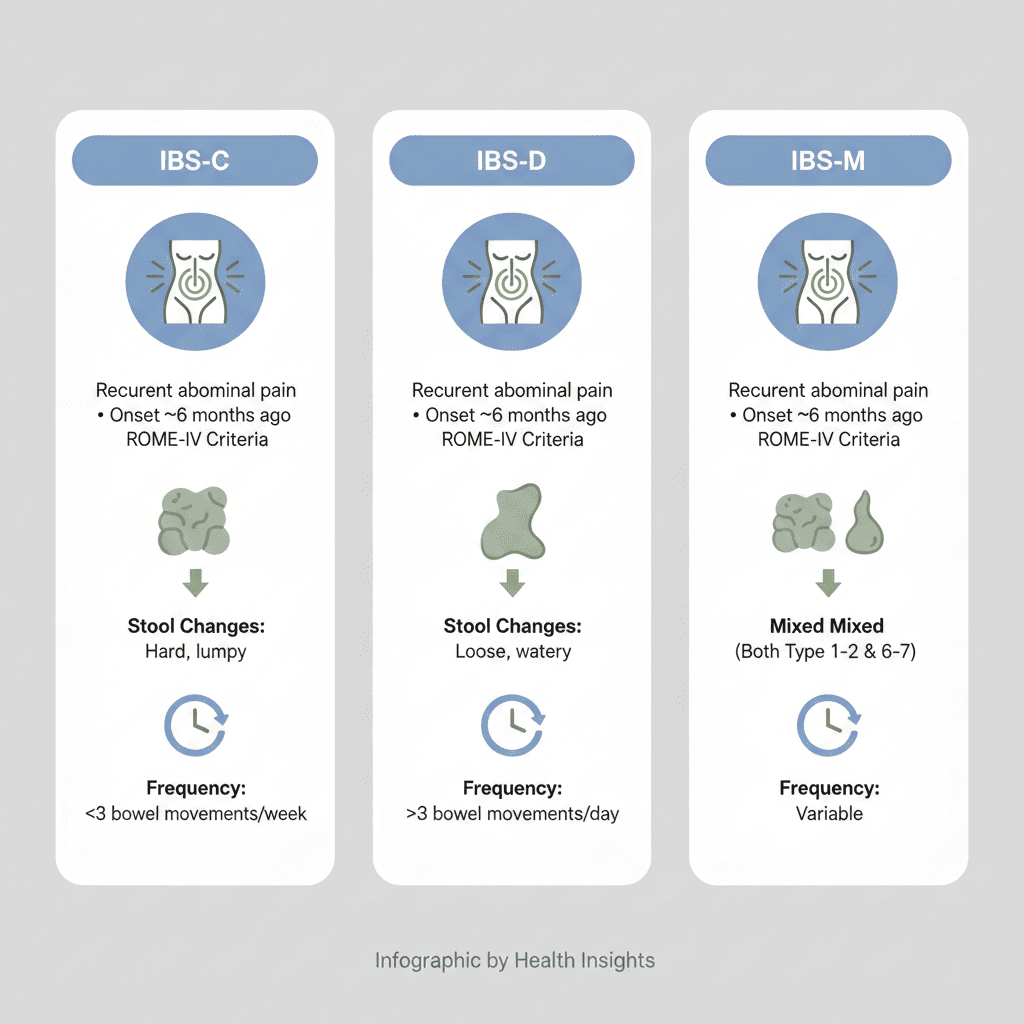
IBS is further classified into three subtypes based on your stool patterns:
Understanding your specific subtype can help guide treatment options, from dietary changes to medications.
The Rome IV criteria provide clear guidelines for doctors to diagnose IBS accurately. Without these criteria, it’s easy to confuse IBS with other conditions that have similar symptoms, such as inflammatory bowel disease (IBD), celiac disease, or even lactose intolerance. Having a structured diagnostic system ensures that patients get the right treatment and avoids unnecessary tests or treatments.
Doctors use the Rome IV criteria in conjunction with other diagnostic tools to rule out other conditions and confirm that IBS is the correct diagnosis.

Diagnosing IBS isn’t just about recognizing IBS symptoms-it’s also about ruling out other potential causes of those symptoms. Many conditions have symptoms that overlap with IBS, such as:
In addition to the Rome IV criteria, doctors may perform tests like blood tests, stool samples, or imaging studies to rule out these other conditions. Once these are eliminated, IBS can be confirmed.

Once IBS is confirmed using the Rome IV criteria, the next step is to create a personalized treatment plan. IBS management usually involves a combination of dietary changes, lifestyle adjustments, and possibly medications.
It’s important to work closely with your doctor to develop a plan tailored to your symptoms and lifestyle.
Understanding the Rome IV criteria can make the process of diagnosing IBS feel less confusing. With these criteria, doctors have a clear way to rule in IBS and rule out other conditions, ensuring that you receive the right care.
IBS can feel overwhelming, but with the right diagnosis and a customized treatment plan, it is possible to manage your symptoms effectively and lead a healthy, fulfilling life.