Stay Updated with Wellness Digestive




No spam, no fluff—just practical, evidence-based advice delivered straight to your inbox every Tuesday.






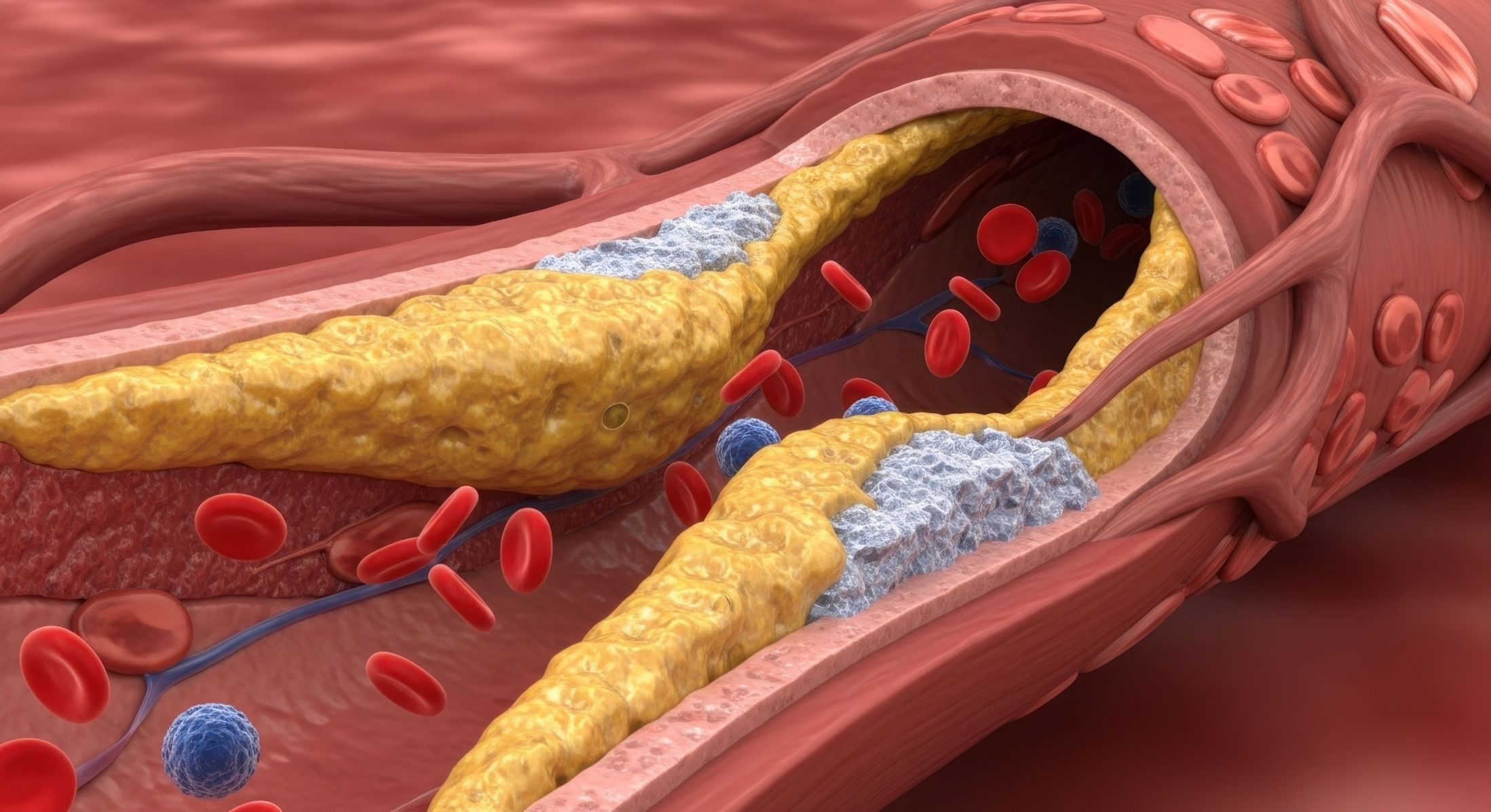
Cardiovascular conditions continue to rank among the most critical challenges in public health today, necessitating cutting-edge investigations to uncover new contributing factors. A groundbreaking study recently featured in Nature has revealed that imidazole propionate, a compound produced by bacteria in the gut, plays a significant role in the onset and advancement of atherosclerosis, positioning it as a promising indicator for detecting subclinical cardiovascular issues before symptoms appear.
Heart and vascular diseases stand as the primary cause of death across the globe, but the complete mechanisms behind their development remain elusive, which complicates the creation of reliable early detection methods and targeted therapies. Even with standard interventions aimed at conventional risks like elevated cholesterol, a substantial number of patients still experience serious cardiac incidents. Growing scientific insights point to persistent inflammation and alterations in the gut microbiome as key players in fostering atherosclerosis, offering opportunities to pinpoint subtle early signs in people who show no outward symptoms.
The latest research published in Nature demonstrates that a specific metabolite derived from the gut microbiota, known as imidazole propionate (ImP), actively promotes the formation of atherosclerosis and could serve as a valuable tool for identifying early, ongoing plaque development in its nascent stages.
Researchers employed an unbiased metabolomics strategy to examine atherosclerosis-susceptible ApoE-knockout (ApoE–/–) mice, a standard model for studying this condition due to their naturally high plasma cholesterol and predisposition to plaque buildup. This screening identified microbial metabolites linked to the initial phases of atherosclerosis, with ImP emerging as a prominent candidate. ImP arises from the bacterial breakdown of histidine in the gut and has previously been connected to conditions like type 2 diabetes, coronary artery disease, and heart failure.
Further analysis revealed elevated ImP concentrations in the blood of participants from two distinct cohorts-one from Spain and another from Sweden-who had subclinical atherosclerosis, when compared to healthy controls. These levels strongly correlated with early disease stages, even after accounting for established risk factors such as body mass index, fasting blood sugar, and hypertension. Notably, individuals exhibiting metabolically active subclinical atherosclerosis, evidenced by heightened uptake of 18F-fluorodeoxyglucose in arterial tissues via imaging, displayed even higher plasma ImP. Incorporating ImP into risk assessment models enhanced the accuracy of predicting cardiovascular danger beyond traditional markers. David Sancho, the lead author, emphasized in a related highlight in Nature Cardiovascular Research: “The clinical importance of this discovery lies in ImP’s involvement at the very outset of the disease. This paves the way for proactive detection approaches, especially for those who might seem low-risk based on standard evaluations.”
To determine if ImP directly causes atherosclerosis, scientists administered it orally to atherosclerosis-prone ApoE–/– mice as well as LDL receptor knockout (Ldr–/–) mice. The results showed that ImP triggered substantial plaque accumulation in the aorta and aortic root across both models, remarkably without any changes to blood cholesterol or glucose levels. Mechanistic studies uncovered that ImP stimulates inflammatory signaling in macrophages and fibroblasts, leading to greater infiltration and proliferation of T cells alongside expansion of pro-inflammatory monocytes. The mTOR signaling pathway was identified as a critical mediator of ImP’s pro-atherogenic effects. Intriguingly, treatment with an antagonist to the imidazoline receptor I1R, known as AGN192403-which is widely expressed in the body-completely halted plaque formation and mitigated disease advancement, even in mice on a cholesterol-enriched diet. The researchers propose that this I1R blockade could synergize with statin-like cholesterol-lowering agents, offering a novel strategy in precision medicine. By modulating microbiome-derived factors, such interventions could effectively address subclinical inflammation and atherosclerosis in apparently healthy populations.
In summary, these discoveries establish ImP as a dual-purpose factor: both a biomarker for detecting early, active atherosclerosis and a causal agent in its progression. The evidence bolsters ImP’s utility in refining disease risk evaluation and patient stratification, providing additional predictive power over classic indicators like LDL cholesterol. Furthermore, targeting the ImP-I1R pathway emerges as a compelling avenue for innovative atherosclerosis therapies, potentially revolutionizing how we approach cardiovascular prevention and management through gut microbiome insights.
This research not only deepens our understanding of how gut-derived metabolites influence vascular health but also highlights the interconnectedness of microbial activity, inflammation, and chronic disease. By focusing on early subclinical phases, where traditional diagnostics often fall short, ImP offers a window into personalized risk assessment. Future studies may explore dietary or microbial interventions to lower ImP production, complementing pharmacological approaches like I1R antagonists. Such multifaceted strategies could significantly reduce the global burden of cardiovascular diseases, emphasizing the need for integrated microbiome-cardiovascular research.