Stay Updated with Wellness Digestive




No spam, no fluff—just practical, evidence-based advice delivered straight to your inbox every Tuesday.






If you have IBS, you’ve probably heard something like: “It’s just stress.” And even if people mean well, that framing can feel dismissive-because what you experience is real: pain, urgency, bloating, constipation, diarrhea, nausea, and the exhaustion of not being able to predict your gut.
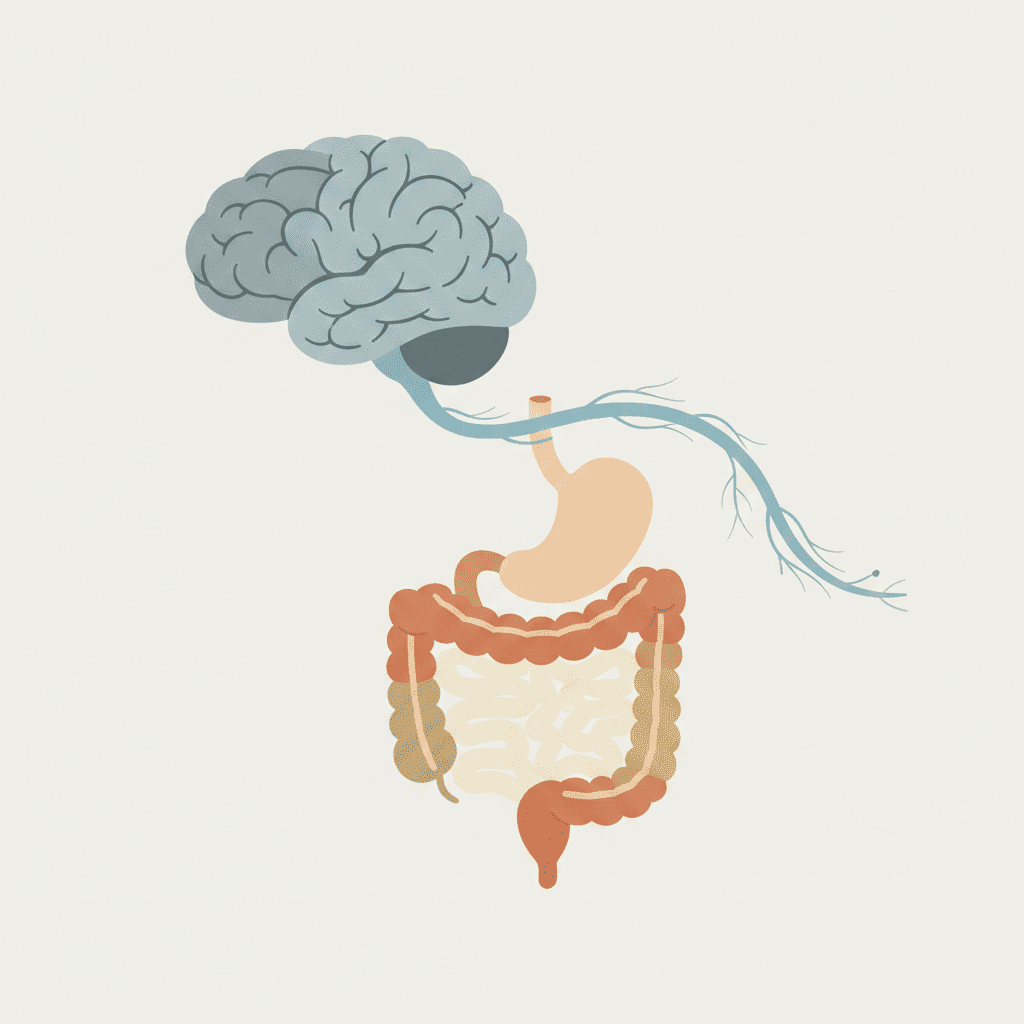
Here’s the truth: stress can trigger real physical IBS symptoms because your gut and brain are wired together-through nerves, hormones, immune signaling, and the microbiome environment. This is called the gut–brain axis.
The gut–brain axis is the two-way communication network between your brain and spinal cord, your autonomic nervous system (fight/flight vs rest/digest), your enteric nervous system (the gut’s “mini brain”), hormone signaling, and immune pathways.
In IBS, this system can become more reactive. That doesn’t mean symptoms are “in your head.” It means the system is more easily activated, and your gut responds more strongly to certain signals.
Your autonomic nervous system has two main branches: the sympathetic (“fight/flight”) and the parasympathetic (“rest/digest”). Under stress, sympathetic activity tends to dominate, shifting resources away from digestion.
That can lead to:
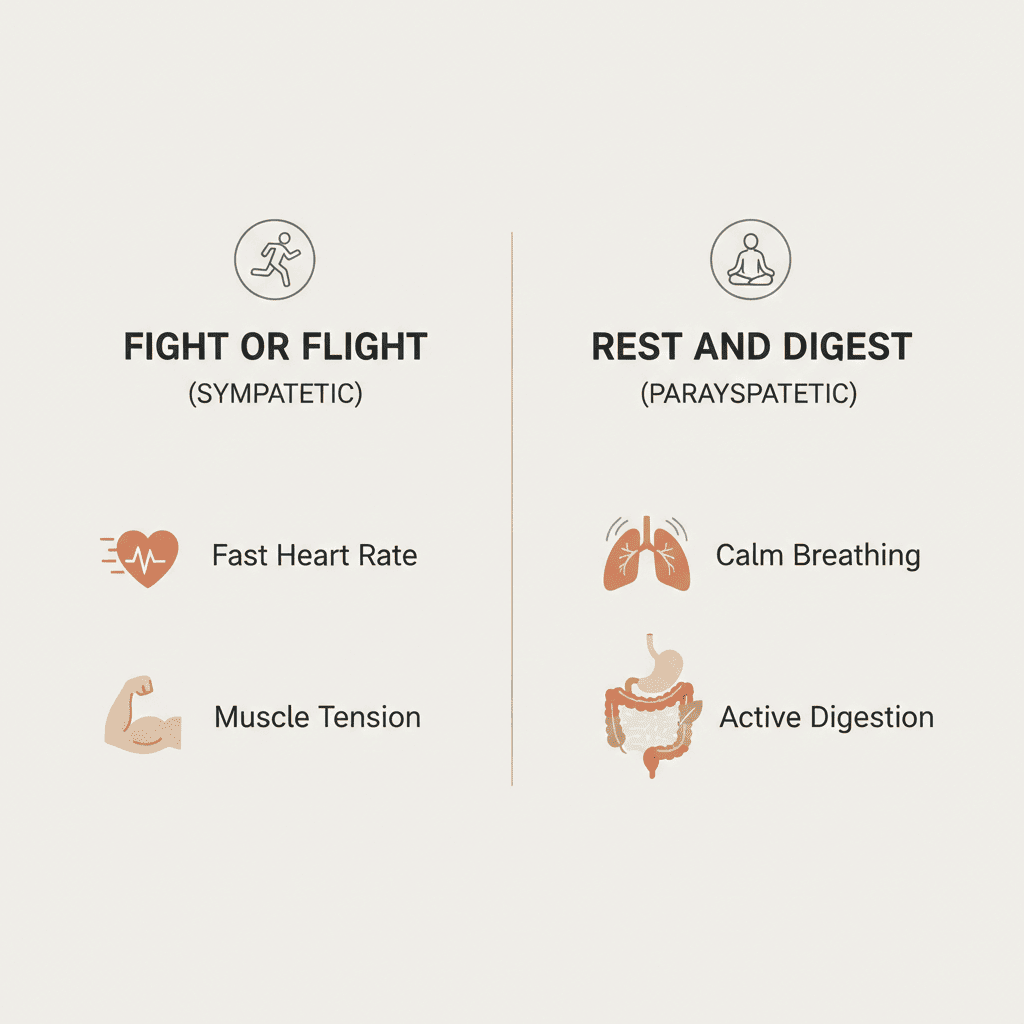

The vagus nerve is a primary nerve connecting the brainstem to the digestive tract. It influences gut motility rhythms, digestive secretions, and inflammatory “tone.” Chronic stress can reduce flexibility in vagal signaling, which can contribute to symptom sensitivity and longer flare recovery.
The HPA axis (hypothalamus–pituitary–adrenal axis) helps regulate cortisol and the stress response. Short-term activation can be useful; repeated activation can affect gut motility, pain sensitivity, immune signaling, and sleep-each of which can worsen IBS symptoms.
This is one reason IBS can feel like a loop: symptoms raise stress, and stress raises symptoms.
A well-described feature of IBS is visceral hypersensitivity, meaning gut nerves can become more sensitive to normal stretching and movement. Stress can amplify this sensitivity by increasing nervous system “gain” and reducing signal filtering.
No. IBS symptoms often come from a stack: a trigger meal, poor sleep, time pressure, dehydration, and recent flare history. A useful question is: “What am I stacking right now?”
Stress can drive IBS symptoms, but it should never be used to dismiss symptoms that need evaluation. Seek medical review for alarm signs such as blood in stool, unexplained weight loss, anemia, fever, persistent nighttime symptoms, or major unexplained symptom changes.
If stress triggers your IBS, your body is responding-not “overreacting.” The goal isn’t to eliminate stress. It’s to build nervous system flexibility so stress doesn’t automatically become a gut flare.